This blog has often dealt with the subject of hydration – rightly so as dehydration is a common problem amongst older people in care homes. It can happen for a large number of factors – physiological ones like the complex neural triggers for thirst declining with ageing or malfunctioning in those with dementia to behavioural ones such as service users attempt to self-manage their incontinence. Dehydration can lead to a number of conditions that may require additional medication – such as constipation, urinary tract infections and headaches. In addition, dehydration may leave service users confused and lethargic.
Dehydration can impact on performance of care home staff
But it is not only dehydration that can impact service users, it can also impact on performance of care home staff. A small study recently undertaken in a Highland care home, and highlighted by Eveleyn Newman (nutrition and dietetics advisor for care homes in NHS Highland), suggested that care home staff are not consuming enough fluid each day.
Care home staff consume less fluid than recommended
The study, carried out through the dietetics department of Robert Gordon University, was undertaken with staff to clarify whether dehydration might be an area of staff health which needed more focus. Staff volunteered to record their total daily intake of fluids over a 3 day period.
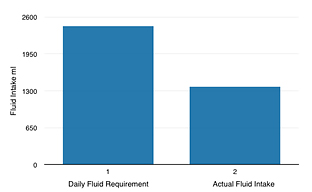
30 – 35ml/kg is a clinical calculation of fluid requirements, for example used in hospitals. European guidelines for average adequate amounts of water are 8-10 glasses a day (1600 – 2000ml). Even considering these average figures, staff still drank considerably less than recommended.
Participants also reported that they experienced the following symptoms of dehydration; thirst, lack of urine, tiredness, inability to concentrate, headache and light headedness.
Reasons in the study given by staff for their intake included:
- “We know we need to drink, but it’s difficult to find the time”,
- “When walking about it’s difficult to carry a drink with you”,
- “Sometimes you make a hot drink, but are distracted by visitors, the phone, then the drink gets cold so you don’t drink it”
The positive outcome of such a study, although small and without strict scientific rigour (for example, no clinical measurements of dehydration were assessed), was that it provided a good way of showing staff that they may not be consuming adequate fluid, and provided an opportunity to highlight the potential benefits from drinking more fluid at work.
It can be easy to forget to drink, but dehydration can have a negative effect on staff health and well-being and may promote symptoms such as tiredness, fatigue and low mood, and contribute to increased staff absence.
Working in a caring environment for vulnerable adults is a demanding role. Adequate hydration is important to help staff perform duties effectively. Dehydration can cause feelings of irritability and a lack of concentration; this could be detrimental to service users.
Encourage adequate hydration in staff and service users
Care home managers and staff should been encouraged to assess their own fluid intake and to take steps within their own care environment to ensure that drinks are encouraged at every opportunity; for example taking tea with residents; having water at staff meetings/handovers; drinking fluids during teaching sessions.
Good fluid intake is also essential for residents and service users too, so support them to have a variety of drinks and flavours; offer fluid rich foods like chilled jellies; soups and milky puddings and use prescribed thickening agents for anyone with dysphagia and in need of texture modification.
Ayela Spiro, British Nutrition Foundation – QCS Expert Nutrition Contributor





