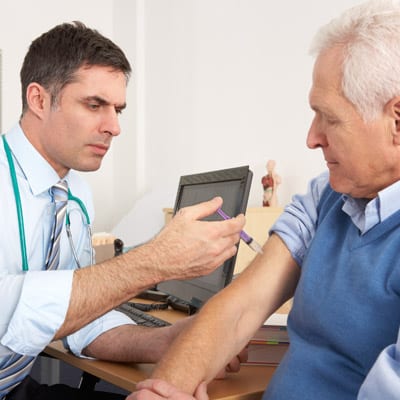
With the flu vaccination season almost upon us, I thought I would highlight the need for – and use – of PGDs. PGDs are the legal mechanism by which a prescription only medicine (POM) can be supplied or administered to a patient for whom no individual prescription exists. All vaccines come under the legal category of POMs. PGDs were introduced through legislation in 2000 and are written agreements for the supply and administration of medicines to groups of patients who may not be identified before presentation for treatment.
What is the difference between a PGD and a PSD?
PGDs can be used for patient groups where general requirements are sufficiently consistent to be provided for by such a non-specific direction e.g. childhood immunisations. A Patient Specific Direction (PSD) is the traditional written instruction, signed by a doctor, dentist, or non-medical prescriber for medicines to be supplied and/or administered to a named patient after the prescriber has assessed the patient on an individual basis. Where a PSD exists there is no need for a PGD. Practices are able to develop their own PGDs if they need to but they must have an agreement with an authorising body such as NHS England or the local Clinical Commissioning Group (CCG).
Who can use PGDs?
We’ve received a few PGDs lately, including the administration of Men C for children aged 2 months to 10 years, and the new Men ACWY vaccine. PGDs can only be provided for specific health professionals and generally includes nurses, midwives, pharmacists, ambulance paramedics, occupational therapists, and dental therapists. Whoever is responsible under the PGD for the supply and administration of medicines must be named on the PGD and this responsibility cannot be passed to others. Implementation of the PGD must be outlined in the specification and only trained and competent staff can administer medicines and vaccines under the PGD.
What should be in a PGD?
Besides the name of the service provider and individuals to whom the PGD applies, other information which should be contained in PGD documentation includes:
- The valid from and expiry date of the PGD
- The medicines to which the PGD applies
- The clinical condition or situation to which the PGD applies
- The criteria for exclusion under the PGD e.g. patient’s aged and medical history
- The description of treatment, including the name, strength and formulation
- The dose and frequency of administration
- The disposal of the medicine
- Any drug interactions, and the management of adverse reactions
Further information about PGDs can be sought from NICE and the RCN.
Alison Lowerson – QCS Expert GP Practice Manager Contributor